| Index to this page |
| Link to discussion of the central nervous system. |
 The peripheral nervous system is subdivided into the
The peripheral nervous system is subdivided into the
| Nerves | Type | Function |
| I Olfactory |
sensory | olfaction (smell) |
| II Optic |
sensory | vision (Contain 38% of all the axons connecting to the brain.) |
| III Oculomotor |
motor | eyelid and eyeball muscles |
| IV Trochlear |
motor* | eyeball muscles |
| V Trigeminal |
mixed | Sensory: facial and mouth sensation Motor: chewing |
| VI Abducens |
motor* | eyeball movement |
| VII Facial |
mixed | Sensory: taste Motor: facial muscles and salivary glands |
| VIII Auditory |
sensory | hearing and balance |
| IX Glossopharyngeal |
mixed | Sensory: taste Motor: swallowing |
| X Vagus |
mixed | main nerve of the parasympathetic nervous system (PNS) |
| XI Accessory |
motor | swallowing; moving head and shoulder |
| XII Hypoglossal |
motor* | tongue muscles |
All our conscious awareness of the external environment and all our motor activity to cope with it operate through the sensory-somatic division of the PNS.
| Link to a discussion of the mechanism by which the commands of the motor neurons of the sensory-somatic system are executed by skeletal muscles. |
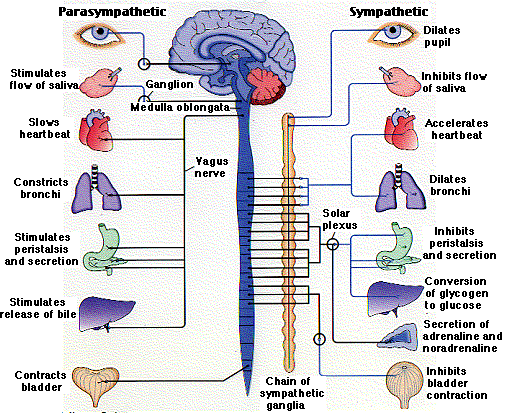
It is responsible for monitoring conditions in the internal environment and bringing about appropriate changes in them. The contraction of both smooth muscle and cardiac muscle is controlled by motor neurons of the autonomic system.
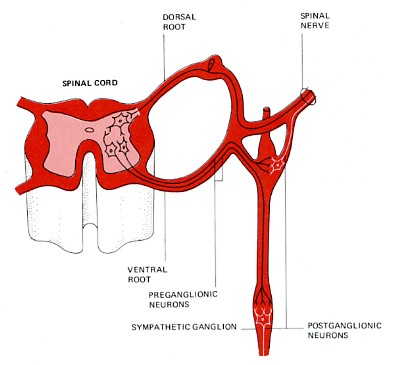
The preganglionic motor neurons of the sympathetic system (shown in black) arise in the spinal cord. They pass into sympathetic ganglia which are organized into two chains that run parallel to and on either side of the spinal cord.
The preganglionic neuron may do one of three things in the sympathetic ganglion:The neurotransmitter of the preganglionic sympathetic neurons is acetylcholine (ACh). It stimulates action potentials in the postganglionic neurons.
The neurotransmitter released by the postganglionic neurons is noradrenaline (also called norepinephrine).
The action of noradrenaline on a particular gland or muscle is excitatory is some cases, inhibitory in others. (At excitatory terminals, ATP may be released along with noradrenaline.)
The release of noradrenalineIn short, stimulation of the sympathetic branch of the autonomic nervous system prepares the body for emergencies: for "fight or flight" (and, perhaps, enhances the memory of the event that triggered the response).
Activation of the sympathetic system is quite general becauseThe main nerves of the parasympathetic system are the tenth (X) cranial nerves, the vagus nerves. They originate in the medulla oblongata. Parasympathetic neurons also extend from three other cranial nerves (III, VII, and IX). Recent work (in mice) indicates that there are no pre-ganglionic parasympathetic nerves extending from the tip of the spinal cord. If this is true for humans, then the bottom-left part of the above figure is incorrect.
Each preganglionic parasympathetic neuron synapses with just a few postganglionic neurons, which are located near — or in — the effector organ, a muscle or gland. Acetylcholine (ACh) is the neurotransmitter at all the pre- and many of the postganglionic neurons of the parasympathetic system. However, some postganglionic neurons release nitric oxide (NO) as their neurotransmitter, and some release noradrenaline.

The Nobel Prize winning physiologist Otto Loewi discovered (in 1920) that the effect of both sympathetic and parasympathetic stimulation is mediated by released chemicals. He removed the living heart from a frog with its sympathetic and parasympathetic nerve supply intact. As expected, stimulation of the first speeded up the heart while stimulation of the second slowed it down.
Loewi found that these two responses would occur in a second frog heart supplied with a salt solution taken from the stimulated heart. Electrical stimulation of the vagus nerve leading to the first heart not only slowed its beat but, a short time later, slowed that of the second heart also. The substance responsible was later shown to be acetylcholine. During sympathetic stimulation, adrenaline (in the frog) is released.
Parasympathetic stimulation causesIn short, the parasympathetic system returns the body functions to normal after they have been altered by sympathetic stimulation. In times of danger, the sympathetic system prepares the body for violent activity. The parasympathetic system reverses these changes when the danger is over.
The vagus nerves carry signals involving many other autonomic actions. Two examples.
In mice, three types of receptors that detect sugar, fat, and amino acids respectively signal the brain (by cholecystokinin, CCK) when food enters the small intestine.
The vagus nerves also help keep inflammation under control. Inflammation stimulates nearby sensory neurons of the vagus. When these nerve impulses reach the medulla oblongata, they are relayed back along motor fibers to the inflamed area. Release of acetylcholine suppresses the release of inflammatory cytokines, e.g., tumor necrosis factor (TNF), from macrophages in the inflamed tissue.
Although the autonomic nervous system is considered to be involuntary, this is not entirely true. A certain amount of conscious control can be exerted over it as has long been demonstrated by practitioners of Yoga and Zen Buddhism. During their periods of meditation, these people are clearly able to alter a number of autonomic functions including heart rate and the rate of oxygen consumption. These changes are not simply a reflection of decreased physical activity because they exceed the amount of change occurring during sleep or hypnosis.
| Link to discussion of the central nervous system. |
| Welcome&Next Search |