The hemagglutination reaction used to determine blood group (A, B, O) is a qualitative test; that is, it simply shows whether antibodies are present or not [View].
However, such tests can be made semiquantitative; that is, provide a number representing the approximate concentration of antibodies in the serum being tested.
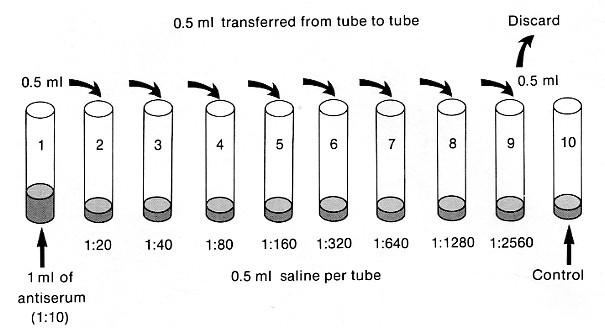
The most common procedure is to add a fixed amount of particles (e.g., red blood cells) carrying antigen on their surface to a series of tubes containing increasing (usually doubling) dilutions of the antiserum. The titer of the antiserum is the reciprocal of the highest dilution in which agglutination occurs.
In passive hemagglutination, red blood cells are agglutinated by antibodies directed against antigens that have been coupled chemically to the red cell surface. Thus the red cell now serves simply as a easily visible indicator of an antigen-antibody interaction.
In the example shown here, the wells in the

Anti-thyroglobulin antibodies are often found in patients with such thyroid disorders as myxedema and Graves' disease
The photograph is courtesy of Dr. C. Lynne Burek.
| Welcome&Next Search |