- a packaging signal (P) needed for the assembly of fresh virus particles
- inverted repeats ("R") at each end; to aid insertion of the DNA copies into the DNA of the target cell.
| Index to this page |
Many human diseases are caused by defective genes.
A few common examples:| Disease | Genetic defect |
|---|---|
| hemophilia A | absence of clotting factor VIII |
| cystic fibrosis | defective chloride channel protein |
| muscular dystrophy | defective muscle protein (dystrophin) |
| sickle-cell disease | defective beta globin |
| hemophilia B | absence of clotting factor IX |
| severe combined immunodeficiency (SCID) | any one of several genes fail to make a protein essential for T and B cell function |
All of these diseases are caused by a defect at a single gene locus. (The inheritance is recessive so both the maternal and paternal copies of the gene must be defective.) Is there any hope of introducing functioning genes into these patients to correct their disorder? Probably.
Other diseases also have a genetic basis, but it appears that several genes must act in concert to produce the disease phenotype. The prospects of gene therapy in these cases seems far more remote.
It is a disease of young children because, until recently, the absence of an immune system left them prey to infections that ultimately killed them.
About 25% of the cases of SCID are the result of the child being homozygous for a defective gene encoding the enzyme adenosine deaminase (ADA). The normal catabolism of purines is deficient, and this is particularly toxic for T cells and B cells.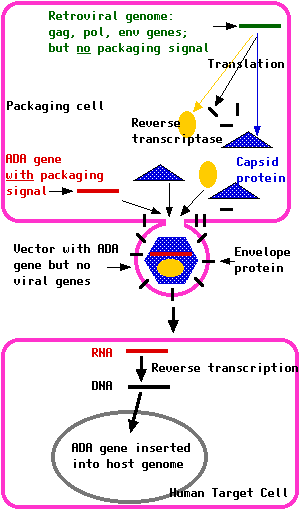 Treated with these two genomes, the packaging cell produces a crop of retroviruses with:
Treated with these two genomes, the packaging cell produces a crop of retroviruses with:Once the virus has infected the target cells, this RNA is reverse transcribed into DNA and inserted into the chromosomal DNA of the host.
The first attempts at gene therapy for SCID children (in 1990), used their own T cells (produced following ADA-PEG therapy) as the target cells.
The T cells were:| But someday there may be a way to make genetically-engineered T cells live indefinitely by getting them to express telomerase. See the discussion. |
| Discussion of blood stem cells |
In June of 2002, a team of Italian and Israeli doctors reported on two young SCID patients that were treated with their own blood stem cells that had been transformed in vitro with a retroviral vector carrying the ADA gene. After a year, both children had fully-functioning immune systems (T, B, and NK cells) and were able to live normal lives without any need for treatment with ADA-PEG or immune globulin (IG). The doctors attribute their success to first destroying some of the bone marrow cells of their patients to "make room" for the transformed cells.
Nine years later (August 2011) these two patients were still thriving and had been joined by many other successfully-treated children most of whom no longer need to take ADA-PEG. These successes led in 2016 to the approval by the European Union of this gene therapy.
Gene therapy has also succeeded for 20 baby boys who suffered from another form of severe combined immunodeficiency called X-linked SCID because it is caused by a mutated X-linked gene encoding a subunit — called γc (gamma-c) — of the receptor for several interleukins, including interleukin-7 (IL-7).
IL-7 is essential for converting blood stem cells into the progenitors of T cells. [View]. Boys with X-linked SCID can make normal B cells, but because B cells need T-helper cells to function, these boys could make neither cell-mediated nor antibody-mediated immune responses and had to live in a sterile bubble before their treatment.
Their doctors*
Five of the little boys developed leukemia (one has died):
|
β-thalassemia is an inherited disease. The most severe cases result from mutations in both copies of the gene encoding the beta chain of hemoglobin. Many causative mutations have been identified, and most lead to a failure to make any beta chains. The resulting hemoglobin functions poorly and the person requires frequent blood transfusions.
In the 16 September 2010 issue of Nature, Cavazzana-Calvo (and many colleagues) report a single case of successful gene therapy for this disorder. Their patient was an 18-year old male.
Their procedure:
The result: Almost three years later, the patient was well and no longer required periodic blood transfusions. One-third of his hemoglobin was now manufactured by the red-cell precursors descended from the gene-altered stem cells.
And using a similar procedure, several babies born with an inherited lysosomal storage disease or Wiskott-Aldrich syndrome (another type of immune deficiency) have, up to two years after treatment with a retroviral vector containing the intact gene, not shown any signs of their disorders (reported in the 23 August 2013 issue of Science).
Another approach avoids the use of a vector by using CRISPR technology instead. During fetal development, the major hemoglobin produced is HbF. It has 2 alpha chains and 2 gamma chains. After birth, it is slowly replaced by adult hemoglobin (HbA) with the same 2 alpha chains but now with two beta chains.
Using CRISPR on harvested blood stem cells of the patient, the enhancer of the BCL11A gene whose product blocks the synthesis of fetal hemoglobin was deactivated. Two negatives make a positive, and when returned to the patient, these cells synthesized HbF and ameliorated the effects of the disease. As of the most recent report (2022), 44 patients in a trial of this technnique are free of disease complications after more than a year.
Children with a particular mutation in both genes encoding the hemoglobin beta chain produce sickle cell hemoglobin, HbS [LINK]
Three methods have shown some success in treating sickle cell disease by gene therapy.In December 2023, the early successes with methods 2 and 3 convinced the U.S. FDA to approve them both — the first CRISPR gene therapies to receive such approval.
Junctional epidermolysis bullosa (JEB) is an inherited skin disorder. In severe cases, the patient's epidermis separates from the dermis forming extensive blisters and exposing the dermis to bacterial infections.
JEB is caused by inherited mutations in one of three genes — LAMA3, LAMB3, and LAMC2 — which encode the 3 subunits of laminin-332. Homozygous mutations reduce or eliminate synthesis of laminin-332 a critical component of the hemidesmosomes that anchor the epidermis to the underlying basal lamina and dermis.
In 2015, a seven-year old boy with a severe case of JEB — caused by a pair of mutant LAMB3 genes — began a trial of gene therapy.
The procedure:Adenoviruses are human pathogens responsible for some cases of the human "cold". Modified versions of two strains are currently being used as vectors in gene therapy trials.
Advantages:Link to discussions of other approaches to gene therapy that are being tried.
|
| Welcome&Next Search |